Latest news and views

Share your feedback to improve care in your community
Share for Better Care, a new campaign launched by Healthwatch and the Care Quality Commission, addresses health inequalities across England.
News

Pharmacists to prescribe drugs for minor illnesses
Pharmacy First scheme will mean patients can get a prescription without needing to see a doctor.
News

New Healthwatch Wiltshire provider announced
After a recent tender process, Wiltshire Council has appointed a new provider for the county’s independent local Healthwatch service.
News


Council continues to provide support during cost of living crisis
With colder weather on the horizon, Wiltshire Council continues to offer a range of information and advice.
News
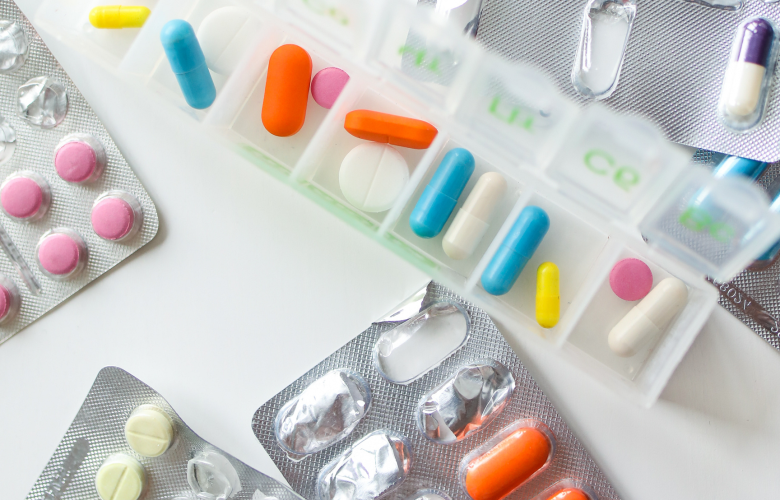
Your feedback on prescription ordering revealed in new report
How people order their prescriptions is the focus of a new report from Healthwatch Wiltshire.
News

Family hubs launching in Wiltshire this April
Families, children and young people will be able to access support both face to face and online with the launch of Family Hubs across the county.
News
New partnership to support unpaid carers announced
Wiltshire Council has announced a new partnership to support unpaid carers in the county.
News
Changes to Prescription Ordering Direct ahead of closure
As part of the gradual winding down of Prescription Ordering Direct (POD), patients in Bath and North East Somerset, Swindon and Wiltshire are being…
News
Latest reports and publication

Quarterly Report January-March 2024
A round-up of our work from the first few months of 2024.
Find out more

Quarterly Report October-December 2023
A round-up of our work from the last few months of 2023.
Find out more